July 12, 2017
Product Update: New MIPS Dashboard | Practice Fusion
If you see Medicare patients, you may be eligible to participate in the Merit-Based Incentive Payment System (MIPS). The Centers for Medicare and Medicaid Services (CMS) estimates that between approximately 600,000 and 650,000 eligible clinicians will be required to participate in MIPS during 2017. By successfully participating in MIPS, eligible clinicians can not only avoid a negative payment adjustment, but can also potentially earn a positive payment adjustment.
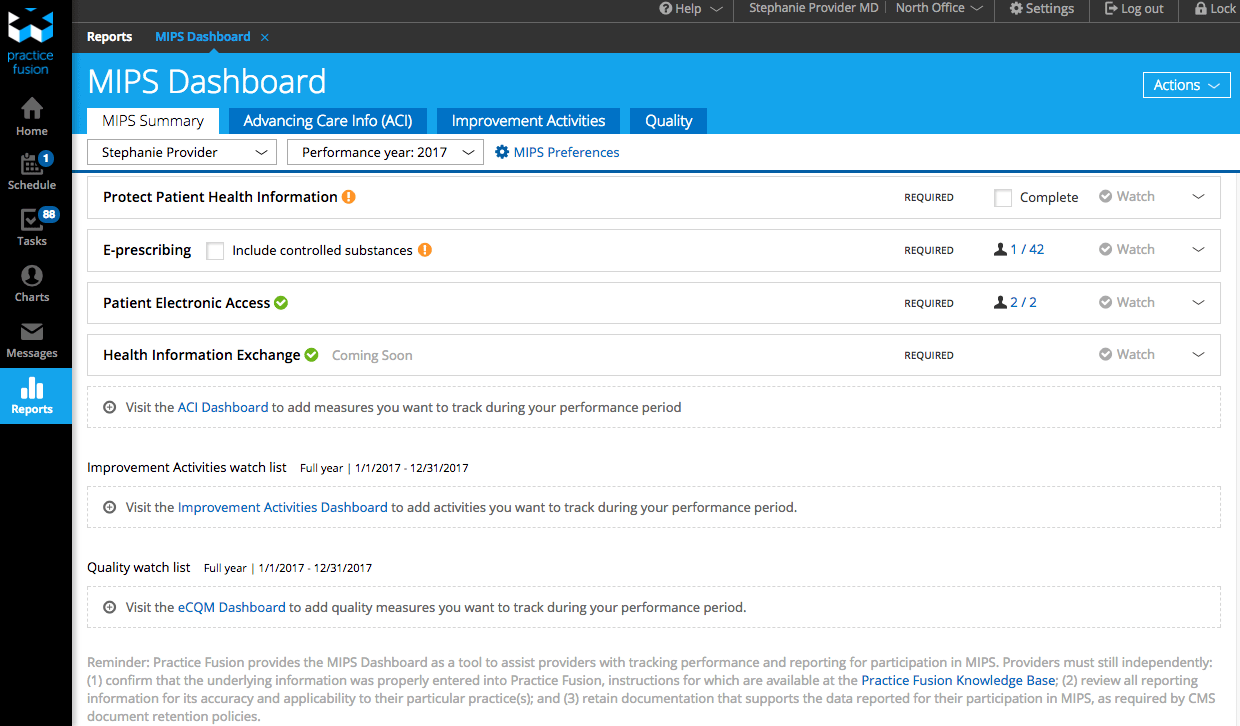
To help you participate in MIPS, we’re pleased to announce that a new MIPS Dashboard is now available in your EHR to help you track your progress. The MIPS Dashboard helps make it easy to track your data in all three MIPS performance categories for the 2017 reporting year. By using the new MIPS Dashboard, you can:
- Learn about each measure. Find out which measures and activities are most relevant to your practice in each performance category under MIPS.
- Select and track your measures. Easily add measures to your MIPS Watch List and start monitoring your performance.
- View MIPS performance benchmarks. See how your performance on MIPS quality measures compares to national benchmarks that will be used to evaluate your performance in 2017 under MIPS.
- Set your participation period. Reporting can easily be toggled between full-year reporting or a custom 90-day reporting period to help you choose the pace of MIPS participation that’s right for you.
- Identify care gaps. Quickly identify patients who may need additional care based on quality measure requirements so you can take action without the need to sift through patient charts.
Get started with the new MIPS Dashboard
Access the new MIPS Dashboard at any time by selecting “MIPS Dashboard” from the Reports section of your EHR.
You can learn more about the MIPS Dashboard by reading our step-by-step guide or attending a Quality Payment Program webinar.
Learn more about MIPS
Practice Fusion is committed to fully supporting your participation in MIPS with new tools, new enhancements, and one-on-one support when you need it.
Visit our MIPS resource page to learn more about the program.
