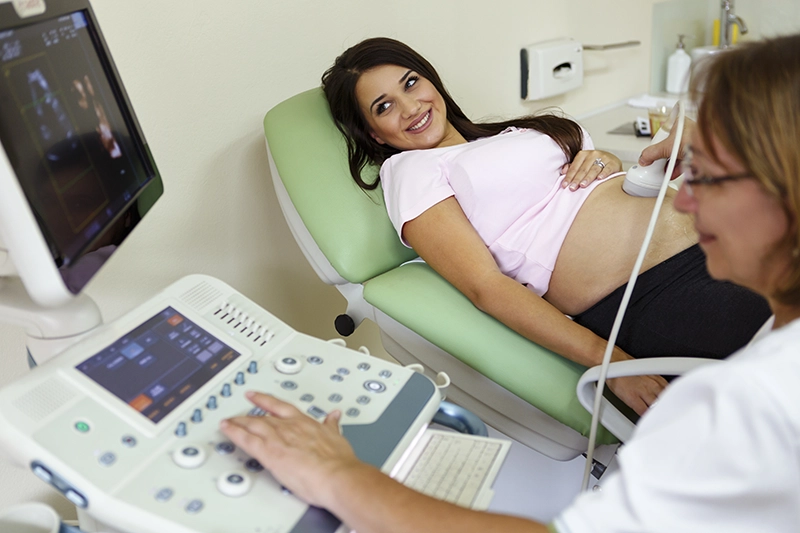
Starting a new practice or switching from paper records?
Whether you are starting a new practice or transitioning from paper charts, Practice Fusion has helped thousands of clinicians transition to a user-friendly electronic health record with fully integrated billing—saving time that can be better spent on patient care.
Meet the EHR and billing services platform that empowers independent practices
Features that help you transition to an EHR

Easy and
Intuitive to Use
Quickly learn just how easy an EHR can be to use, and feel confident every time.

Built for
Independent Practices
Trusted by tens of thousands of independent practices nationwide for over a decade.

Reduce Your
Administrative Workload
Put your patients first by bringing efficiency to your day-to-day operations.
How quickly can you get up and running on Practice Fusion?
With other EHRs:
Your implementation can take
Up to 6-9 months
With Practice Fusion:
You could be charting in
Less than 5 minutes
You could be fully up and running in
2 weeks or less
Let us handle your EHR and billing needs
while you focus on your patients
